relationships

The Secret to Getting Your Dream Wedding on a Budget
Travel
health & fitness

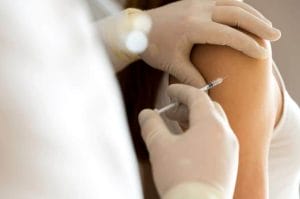
How Businesses Can Slow the Spread of Illness
Discover key strategies for preventing disease spread in the workplace, including educating employees, maintaining clean facilities, and more.
Home & Garden

4 Surprising Radon Facts Everyone Should Know
Radon gas is sometimes called the silent killer because it’s odorless, tasteless, and invisible. Here are a few other facts about this household hazard.
most popular

Patient Care
Ways To Elevate Your Woodworking Techniques

Automotive
How Long Until You Need To Buy a New Car

Home & Garden
4 Surprising Radon Facts Everyone Should Know

Featured Posts, Home & Garden
Virgin Mary Statues: A Touch of Serenity in Pittsburgh’s Gardens
support our advertisers

technology

Debunking Common Myths About Solar Panels
As solar technology becomes more available, more misinformation arises. Learn how to debunk some of the more common myths about solar panels.

Top 3 Features Your Data Center Must Have
What features do you need to have in your data center? The answer is much simpler than you think. Learn how you can implement the best elements here.

Hosting for WordPress
There are a lot of people who are understandably confused by the difference between WordPress.com …

3 Facts About Solar Energy That Might Surprise You
Solar energy is a fascinating scientific field. Without it, the field of free energy would be incomplete. There’s a lot we don’t know. Click here for more.

Reasons Why Every Business Needs a Paper Shredder
Paper shredders are a crucial piece of equipment for any business, big or small. Learn why every business should have a paper shredder available.

5 Things That Can Interfere With Your Wireless Connection
We might think that our wireless internet connection can reach us anywhere, but sometimes that is not true. Here are 5 things that can interfere with it.

The Best Ways To Protect Your Business From Hackers
Hackers are everywhere, targeting everything, and your business is not exempt. Here are some of the best ways to protect your business from hackers.

Recap of the Most Flexible Filaments for 3D Printing
Flexible filaments can have a lot of useful properties for many different types of products. Look here for a recap of the most flexible filaments on the market.

Ways To Protect Outdoor Ethernet Cables
When dealing with Ethernet cables, you must take specific measures to ensure that they’re properly cared for. Follow these steps, and you should have no issues.

Different Data Destruction Techniques You Should Know
Organizing means getting rid of old, outdated records. Here are different data destruction techniques you should know to protect sensitive information.
gift guides

2022 Holiday Gift Guide
The holidays are a time for family, friends, and giving presents! If you’re looking for …

Unforgettable Gifts for Your Mom This Mother’s Day
Mother’s Day is around the corner, and you have just enough time to create the best gift for her. Here are a few gift ideas for Mother’s Day this year.
ENTREPRENEURISM
Using an advanced image upscaler, you upgraded the size and quality of a low-resolution image, resulting in a sharper and more visually appealing picture.